A national consultation and review
Dr Graham Durcan
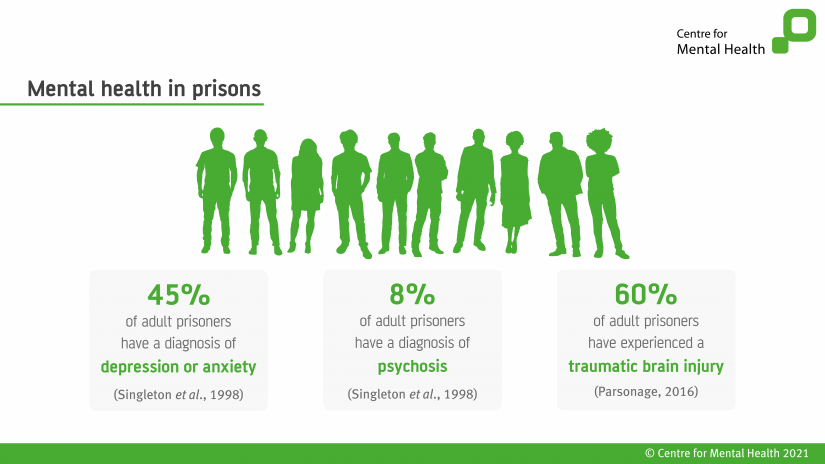
Poor mental health is exceptionally common in prison. 45% of adults in prison have anxiety or depression, 8% have a diagnosis of psychosis, and 60% have experienced a traumatic brain injury. Being imprisoned can exacerbate mental health difficulties, and there are too many avoidable remands and short sentences where a community alternative could have been viable. In recent years prison suicides have reached record levels, and so too have recorded self-harm and violence.
The future of prison mental health care in England was commissioned by NHS England and NHS Improvement, and shares examples of the good and innovative practice happening in prison mental health services. It also finds marked variation in provision from prison to prison, and a paucity of psychological therapy offers in some areas and for some categories of prisoners. Sadly, measures taken to protect people from Covid-19 have exacerbated the risk to mental health in prisons, and opportunities were missed to offer digital support during the crisis. Wider change is urgently needed to improve mental health among people in prison.
The report sets out some key recommendations:
- Make all prisons safer by giving all staff training on mental health and trauma
- Invest in community sentences so that people can get mental health support without going to prison
- Speed up transfers from prison to hospital so that no one waits more than two weeks for urgent care
- Change the Bail Act to stop people being remanded to prison for their ‘own protection’
- Ensure anyone leaving prison with a mental health problem gets health care in their community
- Extend digital mental health support in prison