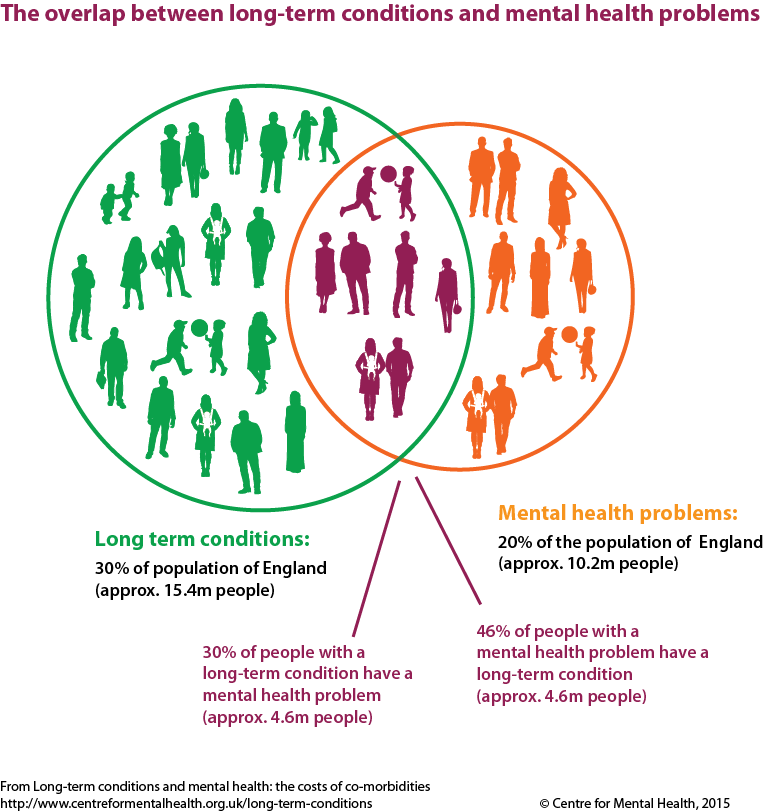
Mental health and physical health are closely interrelated. People living with a physical health problem are twice as likely to have poor mental health, and this can have a detrimental effect on their physical condition.
And many people living with mental health difficulties struggle with their physical health. In fact, people living with a severe mental illness have a life expectancy that’s 15-20 years shorter than those without. That’s why we set up Equally Well UK.
We researched the experiences of people living with severe mental illness of being helped to stop smoking or manage a healthy weight, and heard that few get effective support. For instance, we found that people with severe mental illness are just as keen to quit smoking, but are far less likely to get support to do so. And in terms of healthy weight management, few people with severe mental illness were given support or advice, for instance with managing their weight whilst on anti-psychotic medication. In many cases, people found that there were competing priorities between managing their mental health and managing their physical health.
We have explored how living with a long-term physical health problem (such as diabetes, arthritis, cancer or heart disease) affects people’s emotional health, and what more services should be doing to holistically support people’s health. We worked with National Voices to launch the #AskHowIAm campaign, calling on all health care practitioners to provide compassionate care for people living with long-term physical conditions. And we worked with Kidney Research UK to publish a call to action to improve emotional support to people living with chronic kidney disease.
We have evaluated innovative ways of meeting the needs of people who have complex mental and physical health needs within primary care. These include the Primary Care Psychological Medicine service in Nottingham, which provides psychological support to people with complex needs close to home, working alongside GPs to meet their needs holistically.
All of these pieces of work demonstrate the importance of supporting people’s mental and physical health together, and with equal priority. The traditional divide between body and mind leaves too many people with inadequate or ineffective support. Holistic approaches that combine the two give people a better experience and more chance of recovering, managing their conditions and living well.








